Get to know Dr Jaclyn Wong
DENTAL SURGEON Hawthorn
Dr Jaclyn Wong feels that achieving that perfect smile also involves optimising the framework for your smile. Not only can you rely on premium quality and experienced extraction and implant/All on 4 outcomes, utilising the latest technology in stem cell enhanced soft and hard tissue grafting to ensure optimal aesthetic outcomes, but Dr Wong can also help you with anti-wrinkle injections (DysportTM), fillers (TeosyalTM), BelateroTM and StylageTM), PDO thread lifting and stem cell PRF skin resurfacing therapies.
Her medical, dental and surgical training and a post-graduate diploma in surgical anatomy ensures that treatment is anatomically based and comprehensive. This is crucial to minimising complications and poor outcomes.
Dr Wong will work with her patients to achieve the healthy and long term outcomes they desire, aiming for a natural, rejuvenated and enhanced result. She works in collaboration with Skin Angel for some of these services.
We both practice a less is more philosophy, helping clients to preserve their youthful beauty using natural and effective therapies.
Together we create the perfect conduit between beauty and medicine.


Book an appointment
or ask a question
Leave your details here and a member of our team will be in touch momentarily.
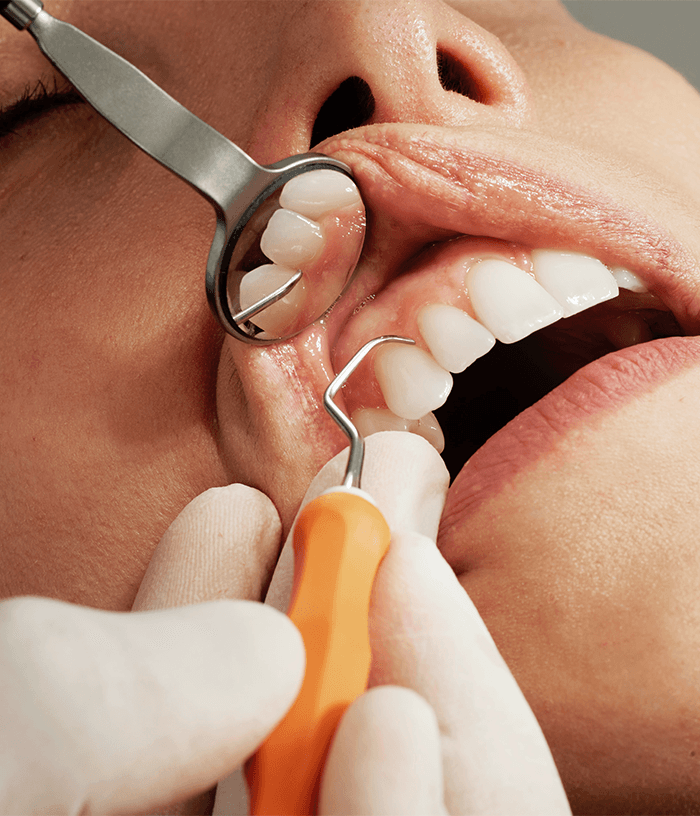
What causes gum disease?
Gum disease is a common problem that can affect people of all ages. It is caused by a build-up of plaque and tartar on the teeth, and can lead to tooth decay, tooth loss and other health problems if left untreated. Read on to find out more about the causes of gum disease, and how it can be resolved…
Gum disease occurs as a result of inflammation in the gums and is most often caused by bacterial infection. The early stage of gum disease is known as gingivitis — if left untreated, gingivitis can become more serious over time and lead to periodontitis, a more serious type of infection.